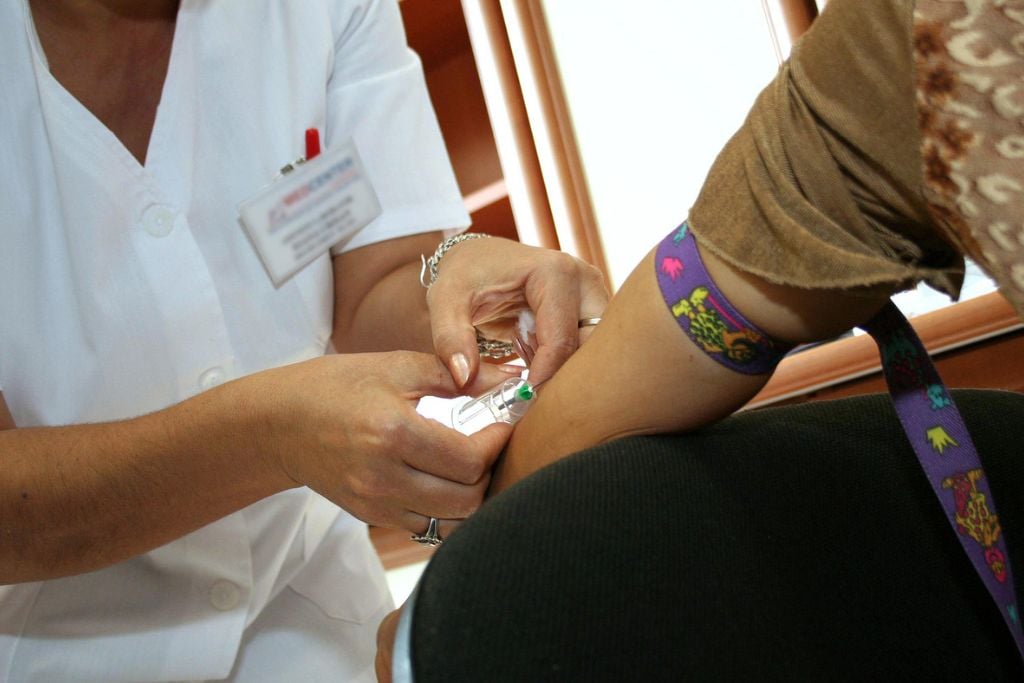
Rapid opiate detox, also known as anesthesia-assisted detoxification, offers a safe and swift path to overcoming opioid dependence for many. The keys to its safety, comfort, and effectiveness lie in the quality of medical resources, the experience of the medical team, and the detox location.
Is Rapid Opiate Detox Safe?
Yes, when experienced anesthesiologists, operating in private ICU rooms of accredited hospitals, conduct rapid opiate detox, it ranks among the most effective treatments for opioid detoxification. This safety and efficacy extend when inpatient recovery care integrates into the treatment plan. Conversely, the risk escalates when providers lack experience or proper credentials, offering quick fixes without a comprehensive care approach. Recognizing the risks and benefits, along with understanding safety measures, medical resources, and choosing the right specialist, is essential.
Why Choose Rapid Detox?
Here are seven reasons why rapid opiate detox under anesthesia is not just safe but also a highly effective choice for those battling opioid addiction. Let these insights guide your or your loved one’s decision towards the most suitable detox path.
1. Minimized Sedation Time Enhances Safety and Eases Withdrawal in Rapid Detox
A key safety feature of rapid opiate detox lies in its short sedation period, typically around 90 minutes or less. This modern approach significantly reduces risks compared to the longer durations of general anesthesia used in the past. Specialists in rapid opioid detox now favor this brief sedation time, minimizing potential complications.
During this time, patients sleep comfortably while their system clears of opiates. Upon awakening, they find themselves better positioned to handle post-detox recovery with markedly fewer withdrawal symptoms.
Waismann Method stands at the forefront of offering this advanced, secure form of rapid opioid detox. Our medical professionals, including a medical director board-certified in anesthesiology, pain management, and addiction medicine, execute the procedure in an accredited hospital setting. Our pioneering medical protocols distinguish our rapid opiate detox as not just safe but supremely effective, setting a new standard in care and patient outcomes.
2. Withdrawal Is Also Shorter After Rapid Opiate Detox
Patients who are candidates for rapid opiate detox tend to not only experience fewer withdrawal symptoms but also shorter durations of opioid withdrawal if any. Use of anesthesia and Naltrexone, an opiate antagonist, during the rapid detox process, means the patient is unaware of the feeling of the opiate being flushed from his or her body, relieving the patient of the burden of withdrawal during that period. With no memory of that part of the process, the patient is freer, physically and mentally, to move through post-detox recovery.
Instead of experiencing painful withdrawal symptoms for a week or more, as can be the case with other treatment options, rapid detox patients generally only experience some withdrawal symptoms for a few hours as their bodies adjust to being free of opioids.

3. Rapid Detox Reduces the Risk of Relapse
In addition to a patient not experiencing most of the unpleasant withdrawal symptoms typically associated with many forms of detox, such as opioid or heroin detox treatment, the patient also wakes up from sedation with little to no opioid cravings because their brain receptors are free and clear of the drug. This process, when combined with Naltrexone therapy and post-detox care such as behavioral therapy, can dramatically reduce the risk of relapse.
4. Medical Care Is Personalized to Address Patients’ Specific Needs
Although rapid detox can be a life-saving procedure for some patients and can dramatically increase patients’ quality of life, it’s not for everyone. Patients’ personal physical and emotional health issues can require treatment plan modifications in order for rapid detox to be as safe and effective as possible.
Patients with Waismann Method®, for example, undergo a comprehensive medical evaluation before their doctor confirms a recommendation for rapid detox. The evaluation includes a comprehensive inpatient assessment and pre-treatment for a full day before anesthesia-assisted detoxification is conducted. Factors examined include the patient:
- Age
- Specific substance abuse or substance dependence history
- Physical health
- Mental health
Based on the assessment of those factors and identification of any specific concerns — such as the patient’s blood pressure and organ function — the patient’s treatment plan is then tailored to their individual needs to increase their success and safety.
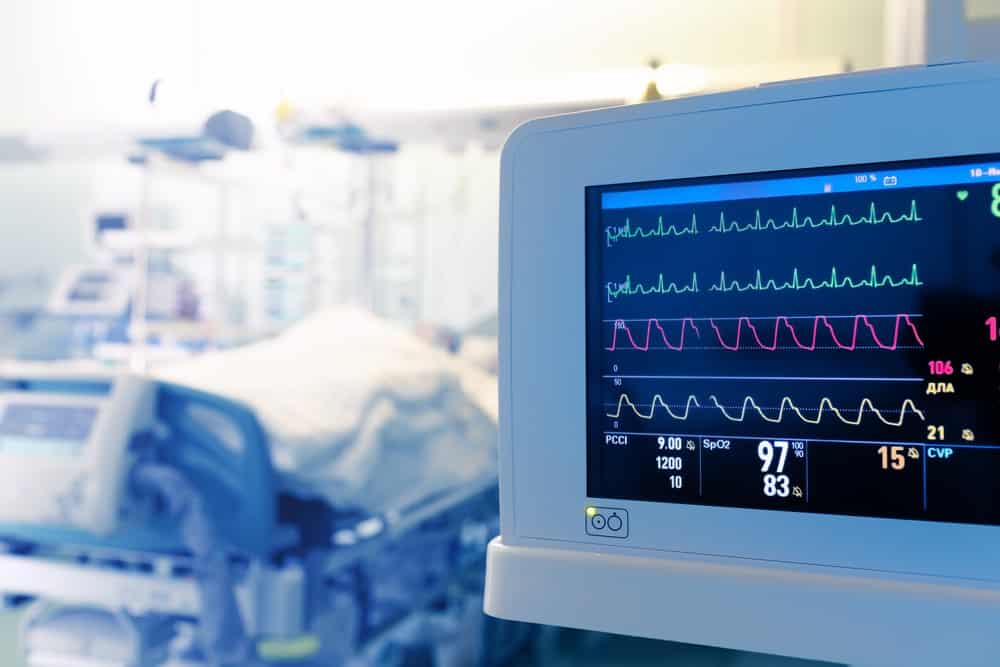
5. Inpatient Care Is Provided in a Private ICU Room to Reduce Patient Risk
Not all rapid detox centers are the same. Some centers provide inadequate medical care and insufficient personal attention, such as:
- They cut the length of inpatient care to inadequate levels in order to fit more patients in.
- They use subpar overnight medical facilities without the necessary immediate medical resources.
- They hire medical providers without the specific experience and training required to perform rapid opiate detox
- They discharge patients to hotel rooms before they are physically ready to leave the hospital.
- They do not provide inpatient or outpatient recovery care.
Such irresponsible practices are why some people misunderstand what rapid detox is and how safe and effective it can be when performed correctly.
Waismann Method®, for example, provides patients with comprehensive care that includes but is not limited to the following:
- Inpatient care is provided in a private, accredited hospital with full medical staff. The patient is given a private room for the procedure in the intensive care unit.
- The hospital and staff are fully equipped with the necessary medical and pharmaceutical resources to handle patients’ needs throughout the rapid detox treatment and post-detox recovery.
- Waismann Method’s medical team has over 20 years’ experience providing rapid opiate detox. The team also offers non-anesthesia detox treatments for patients who are not candidates for rapid detox.
- Patients are not discharged until the medical doctor overseeing the patient’s care deems the discharge date to be safe and appropriate for the patient’s successful recovery.
- Waismann Method patients are discharged to an exclusive aftercare facility, where they are provided with a private suite and post-detox recovery support, such as therapy to assist with sleep, anxiety or other issues.
When researching which rapid opiate detox program is right for you or a loved one, make sure that the treatment includes individualized care in a private ICU room. In addition to the benefits of being in the ICU, a private room provides a safe space for a person to recover in the manner best suited to them instead of being in a room with a stranger. In a private room, the patient can confer with medical staff confidentially, set lighting to their preference and receive the level of attention they need.
ICUs also offer the following benefits:
- Higher staff-to-patient ratio
- Access to medical equipment that isn’t readily available in other medical units
- Emergency medical services, if needed
As with any medical procedure, there is the chance of complications or unforeseen incidents occurring during an anesthesia-assisted rapid detox treatment. But when patients are housed in an ICU during treatment, doctors and other medical staff can respond to these incidents much more quickly than teams that perform rapid detox in other settings. ICUs also don’t have preset discharge times like some treatment or surgical centers do, so patients receive care for the amount of time the supervising rapid detox doctor deems necessary.
6. Rapid Opioid Detox Specialists Are Board Certified and Highly Experienced
Repeated exposure to opioids alters how the brain functions and can cause disrupted breathing, high blood pressure, dehydration, and can impact critical cardiac, pulmonary, kidney, and liver functions. Proper pre-detox assessment and rapid detox treatment needs to be conducted by detox specialists in a full-service, accredited hospital to ensure patient safety.
Additionally, a board-certified anesthesiologist is needed to conduct the anesthesia-assisted rapid detox and to monitor the patient during and after the sedation period. Hospital staff provides support, monitoring patients who undergo rapid detox or alternative, non-anesthesia detoxification. This around-the-clock care by a team experienced in rapid detox treatment ensures that the patient’s recovery is as successful as possible.
Medical professionals who are not specifically board certified or experienced in rapid detox treatment aren’t fully equipped to provide the same level of care as a team like the professionals at Waismann Method, for example. Waismann Method’s team has over 20 years of rapid detox experience, so they understand the specific effects and interactions of opioids and other substances and how to correctly monitor patients before, during and after rapid detox.
Reputable rapid detox centers also have experienced doctors who tailor treatment based on each patient’s individual needs. Waismann Method doctors, for example, are experts in recognizing physical and psychological responses to treatment, so they know how to address various scenarios involving many types of substances and emotional responses to treatment.
Waismann Method’s team also includes a psychotherapist who can support the patient through the post-detox adjustment and recovery phase. The therapist can coordinate with the medical doctor to create a comprehensive treatment that might include medication, if necessary, and can recommend or provide behavioral therapy, stress-management support and other forms of psychological care.

7. Post-Detox Recovery Is Private and Faster
With a rapid opiate detox treatment plan like that provided by Waismann Method, a patient who has undergone the safe rapid detoxification procedure can then be discharged from the hospital to Waismann Method’s exclusive recovery facility. In a private suite at the facility, the patient can safely go through the post-detox adjustment phase with the support of the full Waismann Method medical team, as well as the recovery facility’s staff.
The effects of opioid dependence can cause a person’s body to go through a complex and sometimes exhausting transition after detox. Anesthesia-assisted detox helps to shorten the duration of withdrawal symptoms, but the patient then needs to readjust to what it feels like to no longer have those substances in his or her body. Some patients going through this readjustment phase may experience:
- Discomfort
- Sensitivity to light and temperature
- Erratic emotions
- Anxiety
- Lack of sleep
- Cravings
- Anger
- Depression
Recovery centers like Waismann Method’s Domus Retreat are designed to help patients get through this phase with professional care and attention. Unlike some drug rehabilitation centers, there are no chores or group interactions required, which can seem burdensome or intrusive. Domus Retreat focuses on treating each individual in a serene setting.
This style of post-detox care also contributes to the patient’s successful long-term recovery because the transition phase is handled by professionals instead of well-meaning but inexperienced family members or friends. Spending a prescribed number of days with a professional team equipped with the training necessary to meet the patient’s physical and emotional care needs maximizes the patient’s chances for a full recovery and frees the patient and his or her family and friends from the burden of providing that critical medical care on their own.
Once the patient is through the transitional phase, he or she is then better prepared to take the next steps of focusing on their future. By going through this entire process with the right kind of medical protocols and staff, patients with Waismann Method, for example, have experienced a nearly 100% success rate. Contact Waismann Method’s team to learn more about opiate addiction and opioid dependence treatment methods such as rapid opiate detox and related alternatives.
Published on January 22, 2019
Reviewed by Clare Waismann, CATC, Founder of Waismann Method® Advanced Treatment for Opiate Dependence
All topics for the Opiates.com blog are selected and written based on high standards of editorial quality, including cited sources. Articles are reviewed by Clare Waismann, CATC and founder of Waismann Method®, for accuracy, credibility and relevancy to the audience. Clare Waismann is an authority and expert on opioid dependence, opioid use disorder, substance dependence, detoxification treatments, detox recovery, and other topics covered on the Opiates.com blog. Some articles are additionally reviewed by one of Waismann Method®’s specialists, depending on their field of expertise. For additional information and disclaimers regarding third-party sources and content for informational purposes only, please see our Terms of Service.