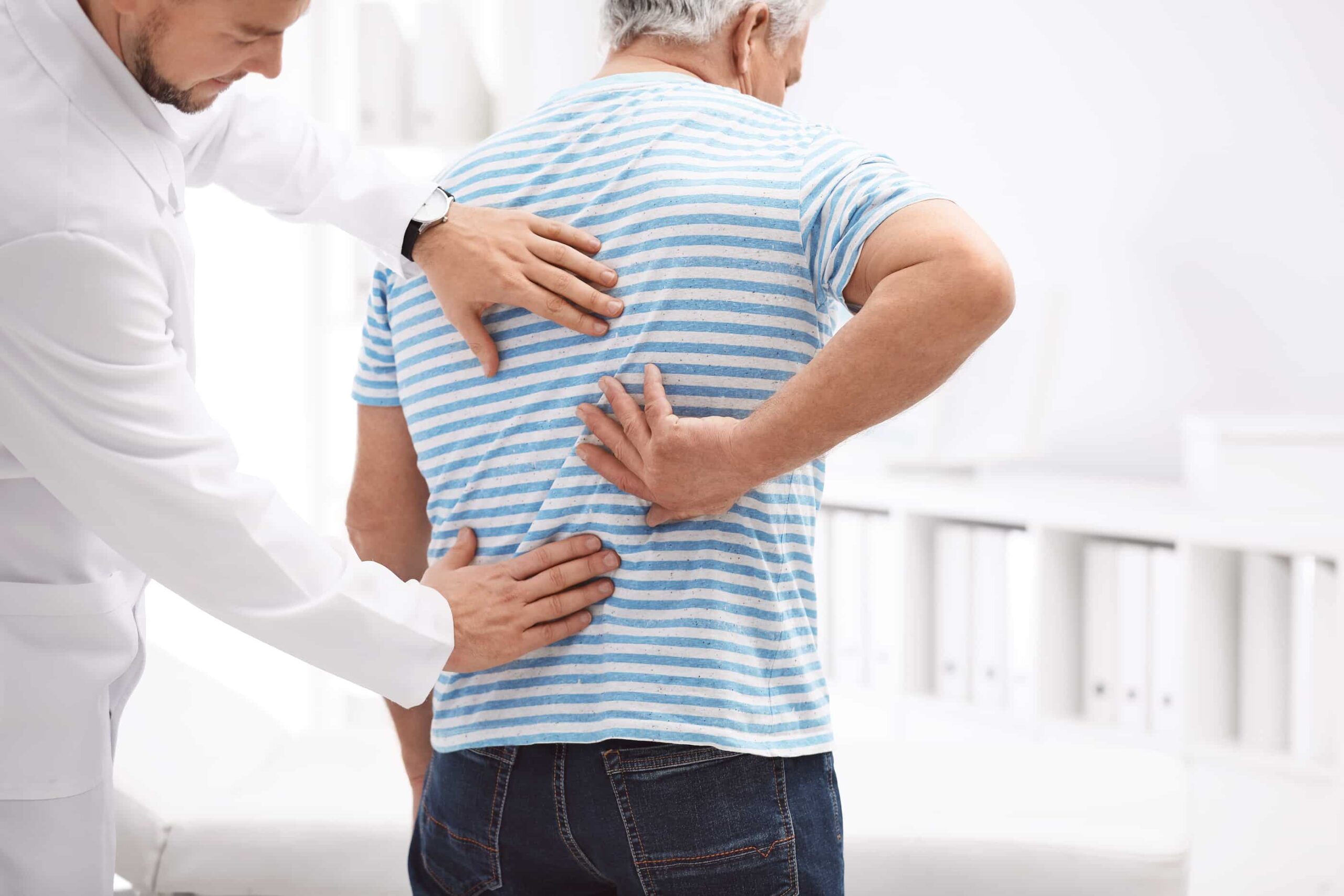
According to the American Psychological Association, the misuse of prescription drugs had risen during the COVID-19 pandemic. People had turned to opioids and stimulants to cope with conditions like anxiety and depression. While these drugs can be helpful when used as prescribed, they can also cause harm if they’re misused. Physicians commonly prescribe opioids to treat pain, yet few people realize that prolonged use of opioids can actually make the pain worse.
A condition called opiate-induced hyperalgesia remains relatively misunderstood by patients and physicians. Here’s what you need to know about hyperalgesia and what you can consider asking your doctor.
What Is Hyperalgesia?
The word “hyperalgesia” means increased (“hyper”) pain (“algesia”). Opiate-induced hyperalgesia is precisely what it sounds like: a condition in which taking opioids causes a person to experience a greater degree of pain.
Read More: What Is Hyperalgesia? Learn the Signs and Symptoms
It is difficult to estimate how many people suffer from hyperalgesia. Experts agree that there isn’t sufficient data to support or refute the condition’s existence and that the quality of available studies on hyperalgesia is poor, according to Practical Pain Management.
Scientists continue to study hyperalgesia, but the exact causes are not yet understood. When a person takes opioids, the opioid molecules bind to special receptors throughout the brain and body. The opioids block pain messages sent to the brain. For some people, after opioids bind, the pain receptors become even more sensitive, meaning as time goes on, even a less-painful stimulus can cause a severe pain response. When this condition develops, the brain receives major pain signals even when the circumstances would normally not be particularly painful.
What Is the Difference Between Hyperalgesia and Tolerance?
Another difficulty patients encounter is understanding the difference between hyperalgesia and tolerance. Tolerance is a normal physiological reaction to taking opioid medications over an extended period of time. As your body becomes accustomed to the presence of opioids, your pain receptors can become less responsive to the drug. This means that you may need a higher dose to achieve the same painkilling effects that you used to get from a lower dose.
Many patients understand that developing a tolerance is a possible consequence of taking opioid painkillers. When some start to experience increased pain, however, they might increase their drug dose to compensate for the tolerance. Taking more opioids than prescribed can be dangerous, so pain patients can benefit from regularly communicating any changes in tolerance to their doctors.
Although patients who have developed a tolerance can still get the painkilling effects of opioids at a higher dose, patients experiencing opiate-induced hyperalgesia feel no effect or pain relief by taking more of the drug. Instead, taking more of the opiate could make things worse by causing pain receptors to become even more sensitized. Complicating things further, patients can experience both hyperalgesia and tolerance at the same time. Disentangling these effects can be challenging, making patient-doctor communication even more critical.
Why Many Pain Patients Are Unaware of Hyperalgesia
Many pain patients have never heard of hyperalgesia and are unaware of its effects. Part of this lack of awareness may be due to physicians failing to mention the possibility of the condition because they think it’s unlikely in their patients.
According to a report on opioid-induced hyperalgesia by physicians at the Institute of Pain Medicine in Haifa, Israel, evidence to support the notion that opioid dose escalation causes OIH is limited, in part because studies of chronic pain patients have used various experimental pain models yielding inconsistent results that can be hard to interpret. The study noted that the need for pain models to establish the clinical diagnosis of OIH — and the need to identify which specific model would be preferred — is yet to be determined.
Some medical practitioners simply write a prescription for opioid painkillers without thoroughly explaining every potential risk. Even if they do describe the risks, doctors may focus on the risk of addiction or developing a tolerance to the medication, not hyperalgesia. Thus, patients may not be informed that they could potentially experience greater pain as a result of taking opioid painkillers.

Why Diagnosing Hyperalgesia Is Important
The lack of studies on opioid-induced hyperalgesia makes it difficult to properly diagnose OIH and means there isn’t data to show how many people are affected by it. And this lack of data means that, even though the condition is a real problem, doctors don’t have evidence or data to make discussing the issue with patients a priority.
The few studies that have been conducted show evidence for hyperalgesia most clearly in patients taking extreme doses, such as opioid abusers and terminal cancer patients with severe pain, according to Science Magazine. Evidence of OIH in patients taking lower doses of opioids over long periods of time, such as when managing chronic pain over months or years, is harder to come by. Variables such as opioid tolerance levels, changes in the underlying condition, or changes in the patient’s chronic pain symptoms complicate diagnosing OIH. Some researchers are working to document changing pain thresholds with quantitative sensory tests to help diagnose OIH, according to Science Magazine.
Risks of Leaving OIH Untreated
Without an abundance of evidence of OIH and a clear method of diagnosing the condition, some doctors remain skeptical of it. Their skepticism can cause them to dismiss a patient’s complaint of excessive pain as an exaggeration. Doctors might even mislabel patients with hyperalgesia as “medication-seeking” if they don’t recognize hyperalgesia as the reason the patients are requesting more drugs.
One of the biggest risks of hyperalgesia going undiagnosed is that physicians might prescribe higher doses of opioid painkillers in an attempt to treat the patient’s pain. This leads to an increased risk of developing or worsening an opioid use disorder. Conversely, if a doctor disregards the patient’s complaints of increasing pain as illegitimate, the patient could be at risk of several problems, such as excessive pain or a potential to use or abuse other drugs in an attempt to relieve hyperalgesia symptoms.
How to Recognize Signs of Hyperalgesia to Discuss With a Doctor
Some physicians are misinformed or underinformed about hyperalgesia, so patients have an opportunity to become their own advocates. People taking opioid painkillers can watch for symptoms of opioid-induced hyperalgesia to consider discussing with their doctor. The most common symptoms include:
- Pain intensity that increases even though the underlying medical condition has not gotten worse
- The area of pain becomes broader than the initially affected region
- New pain develops in a different part of the body without a clear reason or diagnosis
- Formerly painless stimuli now become painful (e.g., light touch or the sensation of wearing clothes may feel painful)
- A change in the quality of the pain, even if it is difficult to describe how the pain has changed
Treatments for Hyperalgesia
The first step in treating hyperalgesia is getting a proper medical diagnosis from a doctor. Patients who suspect they might have hyperalgesia can talk to their prescribing doctors about their questions, pain, symptoms and responses to the medications.
Despite the lack of data currently limiting hyperalgesia research, a study in the Journal of Pain and Palliative Care Pharmacotherapy reported possible opioid and non-opioid treatment regimens for hyperalgesia.
The study’s possible treatment methods involving opioids, such as opioid switching, included using:
- A(2) agonists
- Buprenorphine
- Dextromethorphan (DXM)
- Methadone
Possible non-opioid treatment regimens included using the following:
- Ketamine
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
- Amantadine
Much more research is needed to fully understand, diagnose and properly treat hyperalgesia. Because taking more opioids can make the condition worse, the non-opioid treatment regimens have the potential to be more effective.
How Medical Detox Can Help Treat Hyperalgesia
In order to start a non-opioid treatment for hyperalgesia, a patient would need to stop taking opioid medications. Patients suffering from hyperalgesia, however, might have difficulty with the potential discomfort associated with opioid withdrawal.
A safe, more comfortable and effective way to reverse a physical opioid dependence is medical opioid detoxification. Medical detox dramatically reduces the discomfort and duration of withdrawal. It provides a proven means of safely removing opioids from a person’s pain receptors. Removing the opioids enables their body to gradually return to a normal level of pain response.
Anesthesia-Assisted Detox
Rapid detox is an anesthesia-assisted form of medical detox that can remove opiates from a person’s system in a matter of hours. This procedure, when conducted correctly, is performed by a medical doctor in a full-service, accredited hospital and is highly effective. Waismann Method®, for example, is one of the originators of this procedure. The Waismann team has maintained a nearly 98 percent opioid detox success rate since 1998. The official Waismann Method® is exclusively located in Southern California, treating patients from around the world, and is the only medical detox provider that offers patients a superior combination of medical care and rapid detox experience under the leadership of a medical director who is board-certified in pain management, anesthesia and addiction.
For people managing chronic medical conditions, stopping opioid use might mean needing to find other ways to manage pain. Pain patients can consult their doctors about non-opioid medications and alternative treatments that may be used for pain management, such as:
- Acetaminophen
- Antidepressants
- Gabapentin
- Non-pharmaceutical options like physical therapy, biofeedback and acupuncture
- NSAIDs
For pain patients working with their doctors to find the best treatment options for hyperalgesia and other opioid-related problems, WAISMANN DETOX™ in a full-service hospital can be a viable part of a comprehensive treatment plan. Being treated by a medical doctor who has over 24 years of experience performing the Waismann treatment of medical detox on a range of patients with various complications can provide the peace of mind needed to pursue the next step in opioid-free chronic pain management.
Reviewed by Clare Waismann, Registered Addiction Specialist (M-RAS), Substance Use Disorder Certified Counselor (SUDCC-II), founder of Waismann Method® Advanced Treatment for Opiate Dependence
All topics for the Opiates.com blog are selected and written based on high standards of editorial quality, including cited sources. Articles are reviewed by Clare Waismann, M-RAS/SUDCC II, for accuracy, credibility, and relevancy to the audience. Clare Waismann is an authority and expert on opioid dependence, opioid use disorder, substance dependence, detoxification treatments, detox recovery, and other topics covered on Opiates.com. Some articles are additionally reviewed by one of Waismann Method’s specialists or third-party sources, depending on their field of expertise. For additional information and disclaimers regarding third-party sources and content for informational purposes only, please see our Terms of Service.