No definitive answer currently appears in the literature to answer the question – “Can opiate withdrawal trigger rheumatoid arthritis (RA) flare?” However, we do see related materials about the use of opioid therapy and treatment of RA. Some of this related material can begin to help us answer this question about the effects of opiate withdrawal and triggering such a flare.
The opioid crisis remains a prominent issue in our society. Rheumatologists are at the forefront of this crisis because of the prominent role pain has on patients with rheumatoid arthritis (RA) and the limited treatment options. Physicians continue to discuss the various RA pain mechanisms and available evidence for opioid efficacy and risk for RA patients. They also include a guideline for best practices in opioid prescribing.
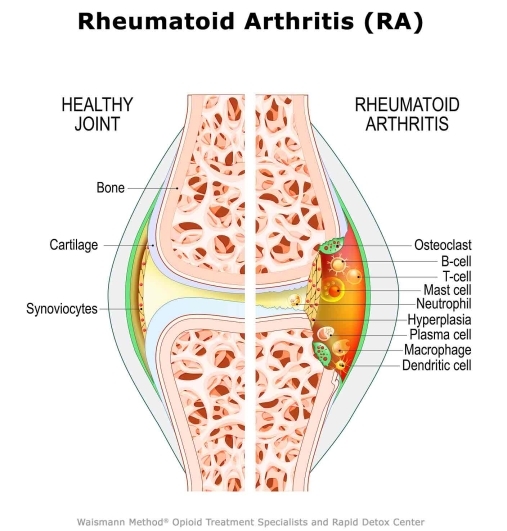
Opioids and Rheumatoid Arthritis (RA)
Whittle et al. in “Opioid analgesics for rheumatoid arthritis pain, “asked the clinical question – Do the benefits of opioid analgesics outweigh the risks in patients who have RA pain? Their conclusion is that a weak opioid might help with the RA pain in the short term. However, “adverse effects are common,” so these adverse effects could outweigh any benefit. The authors infer that “alternative analgesics should be considered first.” These scholars explain what topics are currently being researched concerning opioid use for rheumatoid arthritis treatment.
Another article by Whittle et al., “Opioid therapy for treating rheumatoid arthritis pain,” concluded that limited evidence exists to show low-dose oral opioids can benefit patients with RA. Furthermore, the authors note a possible “offset” for the advantages of using opioids to treat this condition. They also note the evidence is “insufficient” to show conclusions about using low-dose opioids for over six weeks. There is not enough evidence to conclude the use of higher opioid doses either. Furthermore, there is no mention in the study of opiate withdrawal as an RA flare trigger.
Benefits and Risks
Recent studies estimated that nearly 40% of RA patients regularly use opioids. These same studies also conclude that the effects of disease-modifying antirheumatic drugs are minimal in reducing opioid use. Although the literature supports the efficacy of short-term opioid therapy for improving pain, long-term use reduces efficacy while it has the potential of increased safety concerns.
Lee et al., in “Chronic opioid use in rheumatoid arthritis: Prevalence and predictors,” made several important conclusions. First, from 2002 to 2015, chronic opioid use doubled in the United States. Secondly, the “strongest predictors of chronic opioid use” are pain and antidepressant use. They note that research priorities should curb the rise of chronic opioid use. The research should cover strategies for “control of RA disease” and manage depression and pain. Lastly, the authors show again the kinds of issues currently discussed concerning RA and opioid use without addressing opioid withdrawal.
Curtis et al. in “Changing trends in opioid use among patients with rheumatoid arthritis in the United States” also came to some valuable conclusions. The authors concluded a peak in 2010 for opioid use in older patients who had RA. Now, use is declining slightly. Withdrawal in 2010 of propoxyphene from the U.S. market had “minimal effect on overall opioid use.” This is because of an increase in the use of other opioids. The study here aimed to examine trends over time and look at both short-term and long-term use of opioids.
Lee et al. looked at opioid use in RA patients to examine chronic opioid use trends. They intended to determine clinical predictors for opioid abuse. The strongest predictors were pain and antidepressant use. With the rise in opioid use, Lee et al. concluded that research should focus on controlling opioid use for RA patients while managing depression and pain.
Summary
Although the data available regarding opioid use in patients with RA is insufficient, rheumatologists can adhere to best practices and individual patients’ evaluation to determine when and if initiation of opioids is adequate. Identifying the nature of the pain can help determine the suitable treatment course. It is clear that to get a definitive answer to the question – “Can opiate withdrawal trigger rheumatoid arthritis (RA) flare?” – we need additional research.

Clare Waismann is the founder of the Waismann Method and an addiction recovery educator with decades of experience in patient advocacy and program development in collaboration with medical teams. All content is educational only. No medical services are provided.
This content is based on decades of experience in addiction recovery education and collaboration with licensed medical professionals. It is provided strictly for informational purposes and does not constitute medical advice





