Today, we are going to explore a topic that’s unfortunately become all too common in many communities: Opioid Use Disorder (OUD). With millions impacted, understanding OUD is more crucial than ever. So let’s dive right in.
What Exactly is Opioid Use Disorder?
Opioid Use Disorder is more than just a medical diagnosis; it’s a life-altering challenge faced by millions. Characterized by an intense craving and compulsive consumption of opioids, OUD can have far-reaching consequences on both physical and mental health
Defining OUD: Clinical Criteria
The DSM-V, a kind of bible for mental health professionals, helps us define OUD with a range of symptoms. However, at its heart, it’s about a troubling pattern of opioid consumption leading to distress and impairment.
According to data from the CDC, overdose fatalities linked to opioids (encompassing prescription-based opioids, heroin, and synthetic opioids such as fentanyl) in 2021 were a staggering tenfold increase from figures in 1999. In 2021, opioids were implicated in over 80,000 deaths, with close to 88% of these fatalities attributed to synthetic opioids.
DSM requires confirmation of OUD when at least two of the following are present within 12 months:
- Opioids are often taken in more significant amounts or over a more extended period than originally intended.
- A continuous desire, unsuccessful efforts to decrease the dosage, or at least, control opioid use.
- A great deal of concentrating on how to obtain, use, or recover from opioid effects.
- Cravings and urges to use opioids.
- Failure to fulfill primary role obligations due to opioid use.
- Continued use despite having constant problems caused or exacerbated by the effects of opioid use.
- Discontinuation or reduction of social, occupational, or recreational activities because of opioid use.
- Repeated opioid use in physically hazardous situations.
- Opioid use despite the understanding of having persistent or recurrent physical or psychological adverse effects caused or exacerbated by opioid use.
- Presence of tolerance
- Symptoms of withdrawal in case there is a reduction or discontinuation of the drug. DSM excludes those individuals who may experience tolerance and withdrawal, which are taking opioids solely under appropriate medical supervision.
Getting To Know Opioids
Before we delve deeper into OUD, it’s vital to know what opioids are. Primarily, these are drugs designed to interact with our brain, producing pain relief and sometimes, a feeling of euphoria.
Opioids are a class of drugs that bind to specific receptor sites, mostly in the brain. When opioid drugs bind to these receptors, a chemical activation occurs. This activation causes a sense of pain relief and a feeling of euphoria.
Opioid drugs include prescription medications such as morphine and OxyContin, illicit street drugs like heroin and replacement medications such as methadone and buprenorphine. More recently, there has been a deadly influx of synthetic opioids in the United States, mainly fentanyl. Fentanyl is often added to heroin or other street drugs to intensify euphoria and numbing effects. This potent mixture of drugs is continuously responsible for thousands of accidental overdoses.
Why Do People Fall Into The Opioid Trap?
The entrapment in the world of opioids is a complex web, often stemming from seemingly harmless beginnings. For numerous individuals, the path into the opioid abyss begins with a simple, legitimate prescription aimed at alleviating physical pain. However, when the prescribed boundaries of dosage or duration are exceeded, what was once a source of relief transforms into a snare of dependence.
Yet, for another subset of individuals, opioids become an alluring haven, not from physical discomfort but from the haunting shadows of emotional distress or unresolved traumas. For these people, opioids present a temporary solace, a numbing agent to the wounds of the psyche. This dual nature of opioid use, whether as a medical solution or an emotional escape, underscores the multifaceted reasons behind the growing opioid epidemic.
Identifying Opioid Use Disorder: The Hallmark Symptoms
Recognizing the signs of Opioid Use Disorder (OUD) early on can be instrumental in charting a course for effective management and, with the right interventions, eventual recovery. Among the red flags that signal the onset or progression of OUD are:
- Overwhelming Cravings: A powerful and often uncontrollable yearning for opioids.
- Consumption Beyond Control: Despite the best intentions or multiple attempts, an inability to decrease or cease opioid intake.
- Shirking Obligations: Overlooking or entirely abandoning personal, professional, or familial responsibilities due to opioid usage.
- Building Tolerance: The need to increase the opioid dosage to achieve the same effects, indicating the body’s growing accustomedness to the drug.
- Withdrawal Symptoms: Manifesting as nausea, muscle cramping, depression, agitation, and excessive yawning when opioids aren’t taken.
- Risky Behaviors: Using opioids in hazardous situations like driving or operating machinery.
- Social Isolation: Withdrawing from family gatherings, outings with friends, or recreational activities due to opioid consumption.
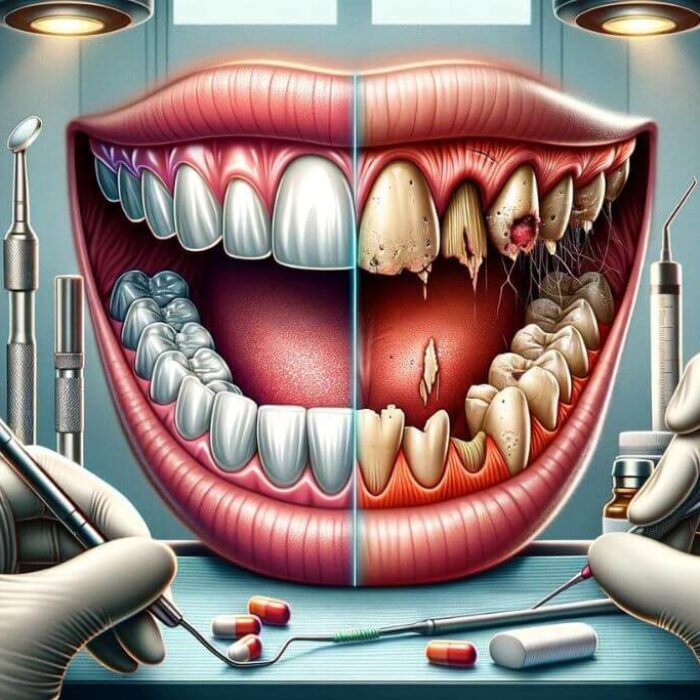
- Physical Deterioration: Neglecting personal hygiene, experiencing unexplained weight loss or gain, and a noticeable decline in overall health.
- Financial Strain: Spending excessive money on obtaining opioids, leading to financial hardships.
- Secrecy and Denial: Hiding opioid use, lying about the quantity consumed, or downplaying its impact.
Being vigilant to these symptoms, especially in loved ones or those around you, can serve as a pivotal step towards intervention and healing.
Navigating the Risks of Opioid Use Disorder
Opioid Use Disorder (OUD) isn’t merely a battle with addiction; it’s a confrontation with a constellation of potentially lethal risks, with the dark shadow of overdose ever-present. But in this foreboding landscape, there’s a silver lining: Knowledge. Armed with the right information, we can protect ourselves and our loved ones, turning a potentially grim narrative into a tale of resurgence and hope.
Understanding the Depths of OUD
In the turbulent seas of addiction, Opioid Use Disorder (OUD) stands out as a particularly menacing wave. Yet, even amidst its challenges, there’s a beacon of hope shining brightly. In the age of information, understanding and leveraging the right knowledge can be our most potent weapon against OUD.
Breakthrough Medications: The New Vanguard Against Opioid Cravings
Pharmaceutical giants have unveiled game-changers in the fight against OUD. Drugs like Naltrexone and Vivitrol are at the forefront, acting as formidable barriers against opioid cravings. With these medications in the arsenal, sustaining sobriety is no longer an uphill battle; it’s a path paved with potent allies.
Waismann Method: The Pinnacle of Opioid Treatments
When it comes to effective OUD treatments, few can rival the Waismann Method. A stalwart in its field, its unparalleled success rates have garnered global attention. By providing a medically supervised and compassionate approach, it offers a lifeline to those grappling with opioid dependence.
Naloxone ( Narcan): The Emergency Lifeguard Amidst the Opioid Crisis
Every minute counts during an opioid overdose, and Naloxone has emerged as the quintessential emergency response. While it’s not the end-all solution, it’s the immediate shield we need against the specter of overdose, buying precious time to seek more enduring solutions.
Journey to Recovery: A Tailored Route to Triumph
Recovery from OUD isn’t a one-size-fits-all approach. It’s a tailored journey, enriched with various treatments—both medicinal and holistic. As individuals navigate their recovery, a multifaceted approach offers the most promising outcomes, bridging the gap between physical well-being and mental fortitude.
To sum it up, the battle against OUD is intense, but it’s far from insurmountable. With strategic treatments, cutting-edge medications, and the power of knowledge, reclaiming life from the clutches of opioids is more attainable than ever. Dive into the resources, empower yourself, and turn the tide in this fight.