
Safe Usage of OTC Drugs: Essential Tips and Guidelines
Welcome to your comprehensive guide on safely navigating the world of OTC (over-the-counter) drugs. In this essential read, we dive into critical tips and strategies
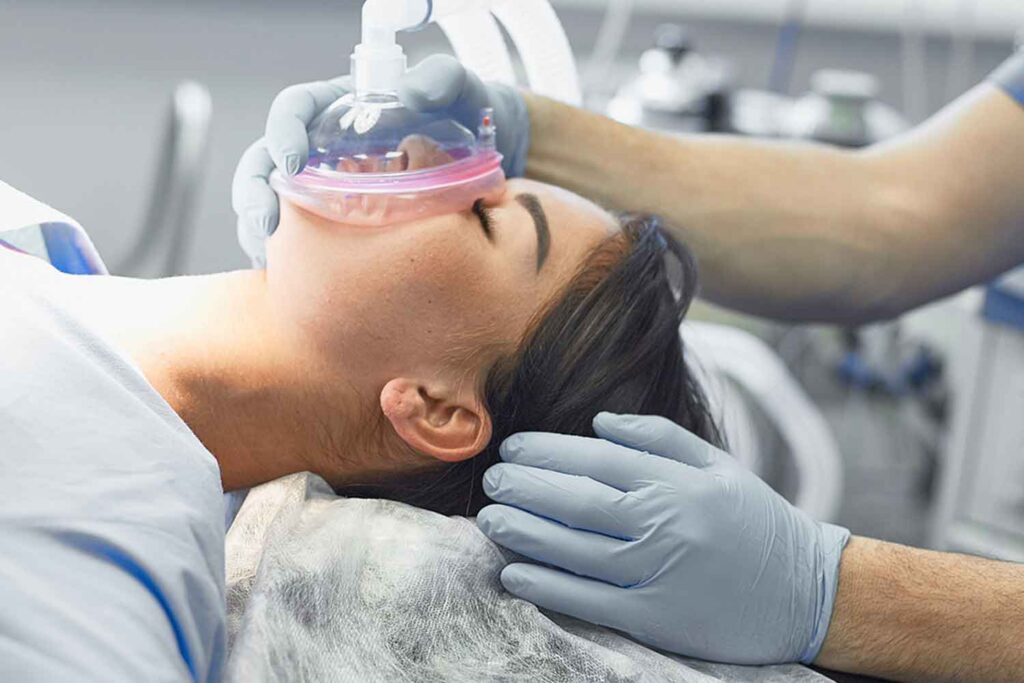
Welcome to the Waismann Method, the nation’s leading provider of anesthesia-assisted opioid detox (also known as opioid detox under anesthesia or sedated detox). This revolutionary method offers a safe and effective path to recovery for individuals struggling with opioid dependence.
Escape Opioid Addiction with the Waismann Method: Safe, Effective Anesthesia-Assisted Detox
Welcome to the Waismann Method, the nation’s leading provider of anesthesia-assisted opioid detox (also known as opioid detox under anesthesia or sedated detox). This revolutionary method offers a safe and effective path to recovery for individuals struggling with opioid dependence.
Imagine waking from a peaceful sleep, free from the physical pangs of opioid withdrawal. Anesthesia-assisted detox makes this possible by utilizing specialized medications and gentle sedation to accelerate the detoxification process. This significantly reduces discomfort and minimizes the potential for relapse.
Ready to reclaim control of your life? Contact Waismann Method today at 1-800-423-2482 to learn more about our life-changing anesthesia-assisted detox program.
Speak Confidentially
with an opiate detox treatment expert.
Opioid dependence can be a formidable challenge, but it doesn’t have to control your life. With the right support and guidance, lasting recovery is possible. Anesthesia-assisted detox can be the first step on your road to a brighter future.
The Waismann Method is built upon a foundation of scientific research and clinical experience. Since the introduction of the “Ultra Rapid Detox” concept in the late 1980s, our team has continually refined and improved the procedure to ensure optimal safety and efficacy.
We believe that every individual deserves access to high-quality addiction treatment. Unfortunately, not all rapid detox programs are created equal. Some prioritize profit over patient well-being, leading to compromised safety standards and inadequate care.
At Waismann Method, we are deeply committed to ethical and responsible practice. We prioritize patient safety and utilize evidence-based protocols to deliver the highest quality care available.
Take the first step towards a healthier, happier life. Contact Waismann Method today to learn more about our revolutionary anesthesia-assisted detox program.
Let’s work together to rewrite your story.
When considering anesthesia-assisted rapid detox for opioid addiction, it’s essential to understand the potential risks, especially if the procedure is not conducted in a fully equipped, accredited hospital. Key concerns include the facility’s ability to handle unexpected issues during detox and having multiple detoxification protocols, with and without anesthesia. This is particularly important for older adults, those with multiple health concerns, or individuals using multiple substances. However, in a hospital setting, these risks are significantly lowered thanks to the presence of specialized medical teams and immediate access to emergency care.
It’s also crucial for opioid detoxification centers to offer a variety of detoxification protocols, tailored to each patient’s specific health needs. The length and approach to treatment should not be one-size-fits-all. Instead, care should be individualized, providing a customized, medically tailored approach to each patient’s unique situation.
Anesthesia-assisted rapid detox presents a safe, effective, and scientifically supported choice for those dealing with opioid addiction, providing an important first step towards a successful recovery.
The benefits of a medically supervised rapid detox under anesthesia are numerous and can make a real difference in your recovery journey:
Anesthesia-assisted rapid detox offers a safe, effective, and scientifically backed option for those struggling with opioid addiction. It marks the first step in your recovery, laying the groundwork for a successful journey to overcoming opioid dependence.
When it comes to choosing a sedated detox program for opioid addiction, the Waismann Method offers an exceptional and comprehensive solution. Alongside our renowned detox method, we also provide exclusive recovery support at Domus Retreat, a key component of our medical approach. Here’s why our program stands out:
National Leader in Opioid Detoxification: The Waismann Method is nationally recognized as the premier provider of medically assisted opioid detox under sedation, leading the field with its advanced techniques and patient care.
Established by an Addiction Treatment Visionary: Founded by Clare Waismann, a registered addiction specialist, our program is built on a foundation of expert knowledge and compassionate treatment.
Unparalleled Medical Expertise: Led by Dr. Lowenstein, with four prestigious board certifications, we offer unmatched medical care. Dr. Lowenstein’s extensive experience in sedated opiate detox has been instrumental in achieving lasting recovery for thousands.
A Global Center for Recovery: Patients worldwide choose the Waismann Method® at our Southern California location, operational since 1998, for its singular focus and consistent high-quality care.
JCAHO Accredited Facility: Our hospital’s accreditation by the Joint Commission on Accreditation of Healthcare Organizations (JCAHO) is a testament to our commitment to the highest safety and care standards.
Domus Retreat: Exclusive Post-Detox Care: Following detoxification, patients transition to Domus Retreat, the only licensed treatment facility specializing in opioid use disorder recovery. This exclusive center offers a few days of specialized care, focusing on physical and emotional healing in a serene and supportive environment.
Choosing the Waismann Method® and Domus Retreat means entrusting your recovery to a program that not only provides medically superior detoxification but also ensures a smooth, supported transition back to health and well-being. It’s a comprehensive pathway to reclaiming your life from opioid dependence.
Sources:
Speak with an Opioid Detoxification Under Anesthesia Specialist Today!
Detoxification at Waismann Method: A Comprehensive and Compassionate Approach to Recovery
What's New at Waismann Method®

Welcome to your comprehensive guide on safely navigating the world of OTC (over-the-counter) drugs. In this essential read, we dive into critical tips and strategies

Substance use disorders (SUDs) and mental health issues share a complex relationship, often intertwining and amplifying each other’s effects. In this blog, we delve into

In the realm of opioid addiction treatment and emergency overdose reversal, Naltrexone and Naloxone stand out as critical medications. Although both belong to the opioid


Get Newsletter Updates from Waismann Method®
"*" indicates required fields
We are available 7 days a week
DISCLAIMER: The text presented on this page is not a substitute for professional medical advice. It is for your information only and may not represent your true individual medical situation. Do not hesitate to consult your healthcare provider if you have any questions or concerns. Do not use this information to diagnose or treat a health problem or disease without consulting a qualified healthcare professional. Be advised that Opiates.com articles are derived from various sources and may not reflect your own country’s regulations.